Add your promotional text...

Revenue Cycle with PMS
Proven Revenue Recovery Outcomes
Our team takes pride in executing an optimized revenue management cycle for your organization by
üProficiently files and tracks appeals to recover lost revenue swiftly.
üTrack uncollected payments making sure no revenue is missed.
üStudy denial trends to decipher repetitive problems and devise effective preventive measures.
üSettle denied claims quickly, curtailing the time spent on appeals and corrections.
üFast-track payment cycles to maintain a steady cash flow.
üWe pin down denial root causes and execute corrective measures to limit future instances.
üRecover underpaid and incorrectly processed claims through detailed payer contract analysis and reimbursement audits.
üCoordinate peer-to-peer reviews and medical necessity consultations with insurance medical directors when required.
üManage high-value AR accounts and complex specialty claims involving:
Oncology
Neurology
Orthopedics
Cardiology
Behavioral Health
Surgical Services
üDeliver detailed denial trend reporting and KPI dashboards to support operational decision-making.
üOptimize payment turnaround times to maintain predictable and healthy cash flow cycles.
üOur clients recover 20% or more within 90 days
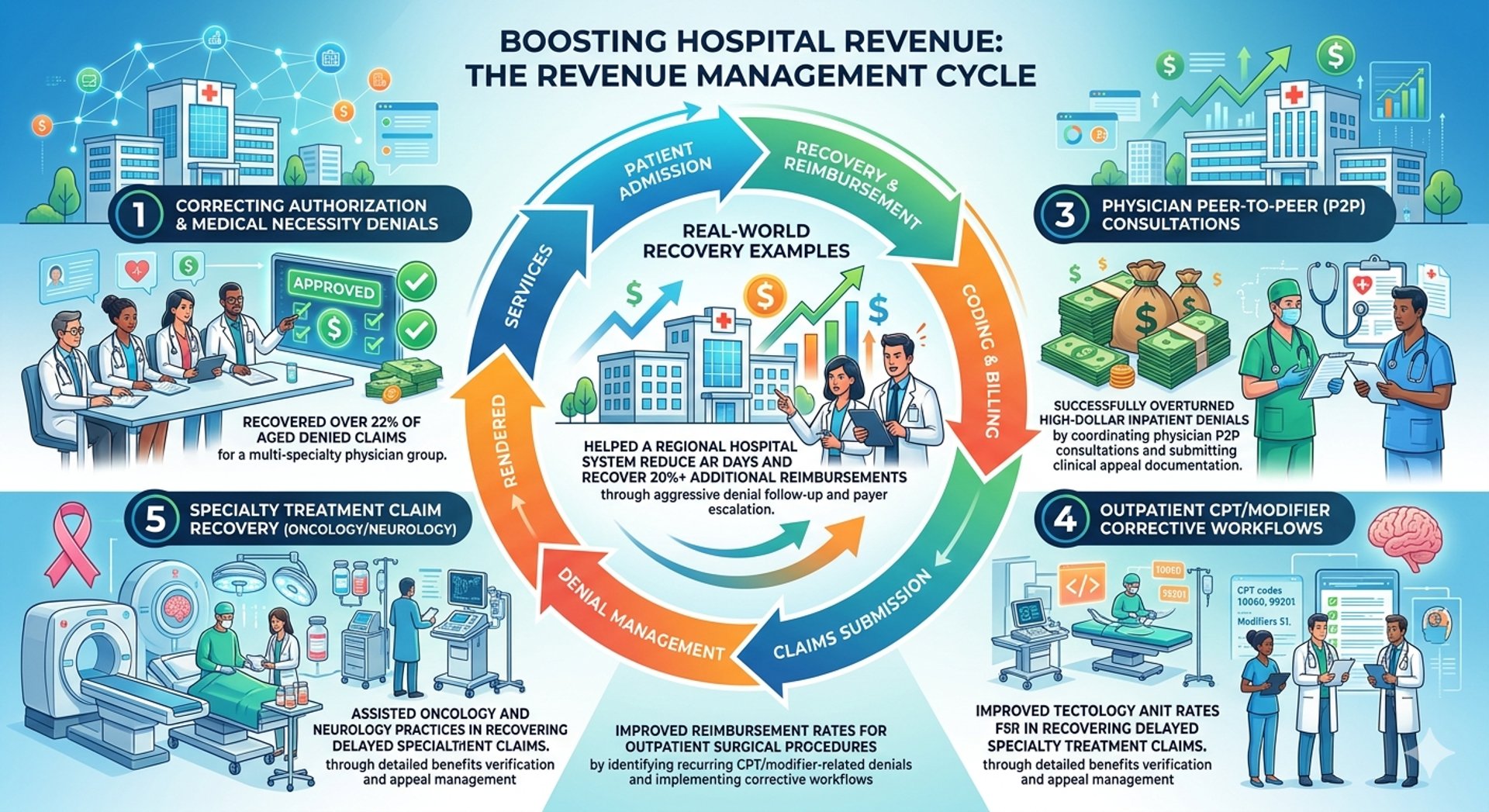
Succes Track Record - Real Examples
ü Recovered over 22% of aged denied claims for a multi-specialty physician group by correcting authorization and medical necessity denials.
ü Helped a regional hospital system reduce AR days and recover 20%+ additional reimbursements through aggressive denial follow-up and payer escalation.
üSuccessfully overturned high-dollar inpatient denials by coordinating physician peer-to-peer consultations and submitting clinical appeal documentation.
üImproved reimbursement rates for outpatient surgical procedures by identifying recurring CPT/modifier-related denials and implementing corrective workflows.
üAssisted oncology and neurology practices in recovering delayed specialty treatment claims through detailed benefits verification and appeal management.
Financial & Operational Benefits
üIncreased net collections and reimbursement accuracy
üReduced claim write-offs and bad debt exposure
ü Lower denial rates and improved first-pass claim acceptance
üFaster revenue realization and healthier cash flow
ü Enhanced payer compliance and documentation accuracy
üReduced administrative burden on in-house billing teams
ü Improved operational visibility through actionable AR analytics & reporting
Prime Medical Solutions combines experienced AR specialists, certified billing professionals, and payer-focused workflows to help healthcare providers maximize revenue recovery while maintaining compliance and operational excellence.

Prime Medical Solutions transformed our practice with their expert support and comprehensive management services. Highly recommended!
Dr. Ayoubi (Onyx Medical Group, FL & TX)

“Team Prime provides outstanding back office & billing support with great attention to detail. Their work has helped us reduce claim delays and improve revenue consistency.”
Dr. Maxwell (Vital Medical Group, Irvine, CA)



